- Home
- About Us
- Work
- Journal
- Contact
- Skidrow sims 4 origin error
- Mac os printer drivers for epson printers
- Shounen onmyouji light novel english translation
- Releasing mac address on android phone
- Windows 3-11 calmira
- Konica minolta printer drivers
- Adobe flash player help for crashing
- Make bootable usb from dmg in windows
- Internet download manager crack file for windows 10
- Endnote add-in word toolbar
- Photorec testdisk ubuntu
- Imaging a mac with munki
- Create bootable linux usb windows 10 for mac
- 1d story of my life mp3
- Btd5 deluxe free download pc
- Export sublime text keyboard shortcuts to vscode
- Divinity original sin 2 crack not opening
- Star plus mahabharat video download
- Percy jackson the lightning thief full movie online free
- Sontham movie writer
- Normal hemoglobin and hematocrit levels in neonates
- Download wirecast for mac
- Native instruments komplete 9 ultimate full download
- Mac pro camera not working
- Free speech to text for pc
- April 2018 monthly planner kit free
- How to uninstall a program on mac osx 10
- Sony vita emulator
- Gran turismo 7 open world
- Best address book software for windows 10
- Any youtube video downloader
- Janet jackson unbreakable tour set list 2017
- Corrupted file recovery software free
- Home
- About Us
- Work
- Journal
- Contact
- Skidrow sims 4 origin error
- Mac os printer drivers for epson printers
- Shounen onmyouji light novel english translation
- Releasing mac address on android phone
- Windows 3-11 calmira
- Konica minolta printer drivers
- Adobe flash player help for crashing
- Make bootable usb from dmg in windows
- Internet download manager crack file for windows 10
- Endnote add-in word toolbar
- Photorec testdisk ubuntu
- Imaging a mac with munki
- Create bootable linux usb windows 10 for mac
- 1d story of my life mp3
- Btd5 deluxe free download pc
- Export sublime text keyboard shortcuts to vscode
- Divinity original sin 2 crack not opening
- Star plus mahabharat video download
- Percy jackson the lightning thief full movie online free
- Sontham movie writer
- Normal hemoglobin and hematocrit levels in neonates
- Download wirecast for mac
- Native instruments komplete 9 ultimate full download
- Mac pro camera not working
- Free speech to text for pc
- April 2018 monthly planner kit free
- How to uninstall a program on mac osx 10
- Sony vita emulator
- Gran turismo 7 open world
- Best address book software for windows 10
- Any youtube video downloader
- Janet jackson unbreakable tour set list 2017
- Corrupted file recovery software free

This is particularly important, for example, with respect to coagulation profiles. Hemoglobin H disease is a good example (in neonates Hb Barts is the abnormal hemoglobin rather than Hb H). Deletion of globin gene, unlike globin gene mutation, causes anemia in neonates.
+..jpg)
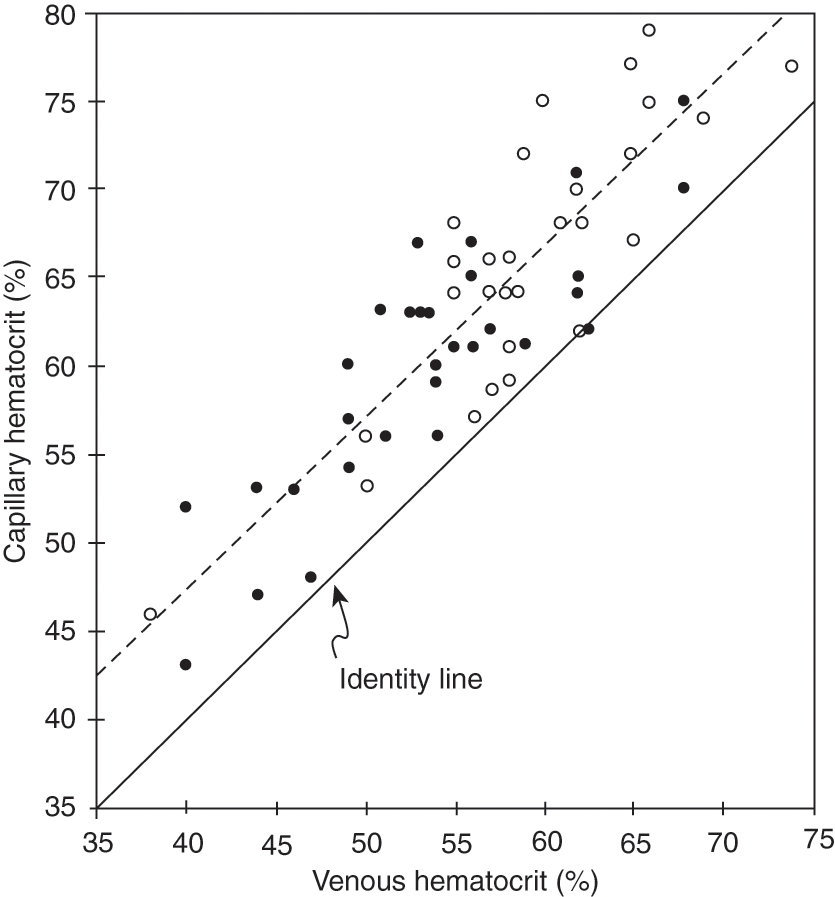
It is always advisable to keep in mind the reference ranges from your own laboratory as they will be analyser or population-specific. Abnormalities of fetal hemoglobin may cause anemia that resolves with the normal shift to adult-type hemoglobins. The calculated minimum acceptable hemoglobin concentration is 6 g/dl for children and adults, 12 g/dl for preterm infants and 11 g/dl for full-term neonates at birth. (100 g per L) and a hematocrit level less than or equal to 30 percentwas. A hemoglobin concentration of 15 g/dl appears optimal for preterm and full-term infants at birth as well as for adults. Is there any risk or danger in correcting an abnormal result? hemoglobin levels is beneficial.1,2 This review.What is the evidence that correcting the abnormality is beneficial?.Is this due to sampling or laboratory error? shifts can alter the hemoglobin and hematocrit levels, and late clamping of the umbilical cord may result in an elevated hematocrit and transitory poly-cythemia.5,6,9 values can vary between sample sites.In most cases, when considering the correction of ‘abnormal’ values, it is wise to consider the following: As (extreme) prematurity is a pathological condition in itself, be cautious when using the concept of ‘normal’. In general, normal pathology values are readily available for healthy term infants. Normal laboratory values are reference ranges used by clinicians to interpret results of laboratory tests. The normal hemoglobin concentration for a term newborn is 19.32.2 g/dL (193220 g/L), with a hematocrit of 617.4 (0.610.074), values that continue to. We recommend that you also refer to more contemporaneous evidence in the interim. The figures presented herein describe reference ranges for hematocrit and blood hemoglobin concentration during the neonatal period, accounting for gestational and postnatal age.Please note that all guidance is currently under review and some may be out of date. During the first 28 days after birth, an approximately linear decrease in hematocrit/hemoglobin occurred.ĬONCLUSIONS. Reticulocyte count: Term Newborn -At birth-3-7 -4th day. During the 4-hour interval after birth, hematocrit/hemoglobin values of late preterm and term neonates (35–42 weeks' gestation) increased by 3.6% ± 0.5% (mean ± SD), those of neonates of 29 to 34 weeks' gestation remained unchanged, and those of <29 weeks' gestation decreased by 6.0% ± 0.3%. Normal Values in Newborn period: Hb and Hematocrit: Term infant ranges from 15.7. No difference was seen on the basis of gender. For every week advance in gestational age, the hematocrit increased by 0.64% and the hemoglobin concentration increased by 0.21 g/dL. In infants younger than 30 weeks gestation, capillary hematocrit values are 20 higher than venous hematocrit. During the interval from 22 to 40 weeks' gestation, the hematocrit and blood hemoglobin concentration increased approximately linearly. those with acidosis, hypotension, and anemia. Data were assembled from a multihospital health care system after exclusion of patients with a high likelihood of an abnormal value and those who were receiving blood transfusions. We sought to develop reference ranges for hematocrit and hemoglobin during the neonatal period (28 days) by using very large sample sizes and modern hematology analyzers, accounting for gestational and postnatal age and gender.
Reference ranges for the hematocrit and the blood hemoglobin concentration of newborn infants have previously been reported from relatively small sample sizes by using measurement methods that now are considered outmoded. “Reference ranges” are developed when it is impossible or inappropriate to establish “normal ranges” by drawing blood on healthy normal volunteers.
